Advances in the Management of Prostate Cancer
Major advances over the last 80 years in diagnosis & treatment (by Professor Roger Kirby)
Once considered a rare disease, now the most common cancer in men
 One hundred and seventy two years ago, Dr J Adams, a surgeon at The London Hospital in Whitechapel, reported a case of prostate cancer. Adams described in his report in the Lancet in 1853 “a case of scirrhous of the prostate gland with corresponding affliction of the lymphatic glands in the lumbar region and in the pelvis" adding that this condition was “a very rare disease”.
One hundred and seventy two years ago, Dr J Adams, a surgeon at The London Hospital in Whitechapel, reported a case of prostate cancer. Adams described in his report in the Lancet in 1853 “a case of scirrhous of the prostate gland with corresponding affliction of the lymphatic glands in the lumbar region and in the pelvis" adding that this condition was “a very rare disease”.
More than a century and a half later, prostate cancer has developed into a major health issue worldwide. In the United States, for example, it is the most commonly diagnosed cancer in men, with around 31,000 deaths occurring annually. In the UK more than 12,000 men die every year from prostate cancer.
 Eighty years ago, the typical prostate cancer sufferer was a man in his early seventies who presented with metastases to bone and/or soft tissues. Characteristically at this time, these tumours were bulky and histologically poorly-differentiated. The prognosis of such an advanced disease status was dire, with the majority of patients dying within a couple of years. The prognosis changed dramatically in the 1940s when Charles Huggins (right) in Chicago discovered that metastatic prostate cancer responded to androgen-ablation therapy; this heralded the beginning of a new era of prostate cancer therapy. Medical castration with oral oestrogens became the first effective, systemic treatment for any cancer, and to this day, androgen ablation remains the most useful and generally applicable prostate cancer therapy. Huggins was awarded the Nobel Prize in Physiology and Medicine in 1966.
Eighty years ago, the typical prostate cancer sufferer was a man in his early seventies who presented with metastases to bone and/or soft tissues. Characteristically at this time, these tumours were bulky and histologically poorly-differentiated. The prognosis of such an advanced disease status was dire, with the majority of patients dying within a couple of years. The prognosis changed dramatically in the 1940s when Charles Huggins (right) in Chicago discovered that metastatic prostate cancer responded to androgen-ablation therapy; this heralded the beginning of a new era of prostate cancer therapy. Medical castration with oral oestrogens became the first effective, systemic treatment for any cancer, and to this day, androgen ablation remains the most useful and generally applicable prostate cancer therapy. Huggins was awarded the Nobel Prize in Physiology and Medicine in 1966.
In 1971, Dr Andrew Schally (right) determined the structure of the hypothalamic hormone known as luteinizing hormone (LH)-releasing hormone (LHRH) and developed the means to synthesize it, creating synthetic peptide agonists of LHRH.
 Schally & his colleagues in 1977 showed that advanced prostate cancer patients who were treated with daily doses of the LHRH agonists experienced a 75% decrease in serum testosterone levels, a decrease or normalization of plasma acid-phosphatase levels and, significantly, a marked reduction in cancer-associated bone pain. Schally received the Nobel Prize in Physiology and Medicine for this ground-breaking work.
Schally & his colleagues in 1977 showed that advanced prostate cancer patients who were treated with daily doses of the LHRH agonists experienced a 75% decrease in serum testosterone levels, a decrease or normalization of plasma acid-phosphatase levels and, significantly, a marked reduction in cancer-associated bone pain. Schally received the Nobel Prize in Physiology and Medicine for this ground-breaking work.
However, the realisation that androgen ablation is seldom curative in the longer term led to two alternative approaches to the treatment of prostate cancer:
- improving the outlook for advanced desease using radiotherapy & chemotherapy; and
- pursuing early diagnosis by developing methods of identofying cancers whol;e they are still confined to the prostate and potentially treatable by definitive local therapy.
Radiation therapy
The first reports on the use of radiation to treat localized prostate cancer appeared at the beginning of the twentieth century and were limited to the introduction of radium sources into the urethra and rectum as a palliative alternative to surgery.
Eventually, prostate tumour growth was slowed by the insertion of radium-containing needles into the prostate gland itself, via the perineum, the rectum or the open bladder. These techniques, however, were difficult to perform and uncomfortable for the patient.
Local irradiation (brachytherapy)
The real interest in brachytherapy did not occur until the 1970s, when Dr Willet Whitmore described an open implant technique using the 125I radioisotope of iodine. Brachytherapy had emerged as a useful approach in some patients with localized prostate cancer.
External beam radiotherapy (EBRT)
EBRT was initially used only as an adjunct to interstitial radium because the kilovoltage delivery systems were not adequate to allow definitive treatment of the most deep-seated neoplasms such as prostate cancer. With the discovery of androgen-ablation therapy in the early 1940s, radiation therapy lost popularity as a treatment for prostate cancer.
 However, interest in radiation therapy returned in the 1950s when higher-energy cobalt machines that could penetrate to deeper levels became available. The first reported series of prostate cancer patients treated with 60Co (cobalt) therapy focused on patients with unresectable disease. In the late 1950s, pioneering work by Malcolm Bagshaw (right) and others confirmed the real possibility of cure of prostate cancer by radiation therapy.
However, interest in radiation therapy returned in the 1950s when higher-energy cobalt machines that could penetrate to deeper levels became available. The first reported series of prostate cancer patients treated with 60Co (cobalt) therapy focused on patients with unresectable disease. In the late 1950s, pioneering work by Malcolm Bagshaw (right) and others confirmed the real possibility of cure of prostate cancer by radiation therapy.
Over the ensuing decades, higher-energy accelerators and new types of radiation were developed. Improved radiographic and data-processing capabilities, such as computerised tomography, resulted in three-dimensional conformal treatment plans that allowed the prostate to be treated with a high dose of radiation, whilst sparing the surrounding normal tissues. In the 1960s, cytoreductive hormonal therapy was added to radiation therapy to reduce tumour burden and provide a more favourable geometry for external irradiation treatment and EBRT.
Prostatectomy for cancer
 In 1867, Theodor Billroth in Vienna performed the first partial prostatectomy via a perineal access. The first suprapubic prostatectomy in Britain was performed in the General Infirmary at Leeds on 24 March 1887 by Arthur Fergusson McGill.
In 1867, Theodor Billroth in Vienna performed the first partial prostatectomy via a perineal access. The first suprapubic prostatectomy in Britain was performed in the General Infirmary at Leeds on 24 March 1887 by Arthur Fergusson McGill.
However, there was no systematic technique for removal of the prostate until the pioneering work of Hugh Hampton Young (right), who, in 1904, at the Johns Hopkins Hospital, performed the first radical perineal prostatectomy.
The next significant surgical advance came in 1945 when Terence Millin in London introduced the retropubic approach for prostate enucleation. This approach offered significant advantage over the perineal approach, because it was easier to learn and also allowed ready access to the pelvic lymph nodes, which is useful for tumour staging.
"Leiden - Drawing Neurovascular bundle of prostate - no labels" by Bas (S) Blankevoort, LUMC and Marco C DeRuiter, LUMC, license: CC BY-NC-SA
Although minor improvements in technique were made over the next 40 years, prostatectomy was not commonly performed because almost all patients were left impotent, and some incontinent, by the  procedure. A significant advance occurred in 1983 when Patrick Walsh (right) developed a modified technique for radical retropubic prostatectomy - on the basis of an anatomical approach - to enhance control of bleeding. This approach reduced injury to the neurovascular bundles adjacent to the prostate that innervate the corpora cavernosa of the penis, thereby allowing erectile function and sexual potency to be preserved without compromising the adequacy of surgical margins.
procedure. A significant advance occurred in 1983 when Patrick Walsh (right) developed a modified technique for radical retropubic prostatectomy - on the basis of an anatomical approach - to enhance control of bleeding. This approach reduced injury to the neurovascular bundles adjacent to the prostate that innervate the corpora cavernosa of the penis, thereby allowing erectile function and sexual potency to be preserved without compromising the adequacy of surgical margins.
Prostate-specific antigen (PSA)
Around the time of the development of this new surgical technique, prostate-specific antigen (PSA) was reported to be a useful serum marker for prostate cancer. Additionally, in the late 1980s, transrectal ultrasound-guided biopsy allowed for high-quality prostate core biopsies to be obtained. These biopsies could be graded according to the Gleason method to either grade 6 (well-differentiated) grade 7 (moderately well differentiated) or 8-10 (poorly differentiated).
These new diagnostic techniques, coupled with improved surgical techniques, led to a dramatic increase in the number of prostate cancer patients who were treated by surgery. The subsequent development of 3T MRI further enhanced the accuracy of diagnosis and staging of localised disease and the adoption of transperineal biopsy has reduced the infection rate of prostatic biopsy.
21st century radical prostatectomy
In the 1990s, laparoscopic radical prostatectomy was introduced and, a decade later, Mani Menon pioneered the use of the Da Vinci robot (below) to facilitate the procedure.
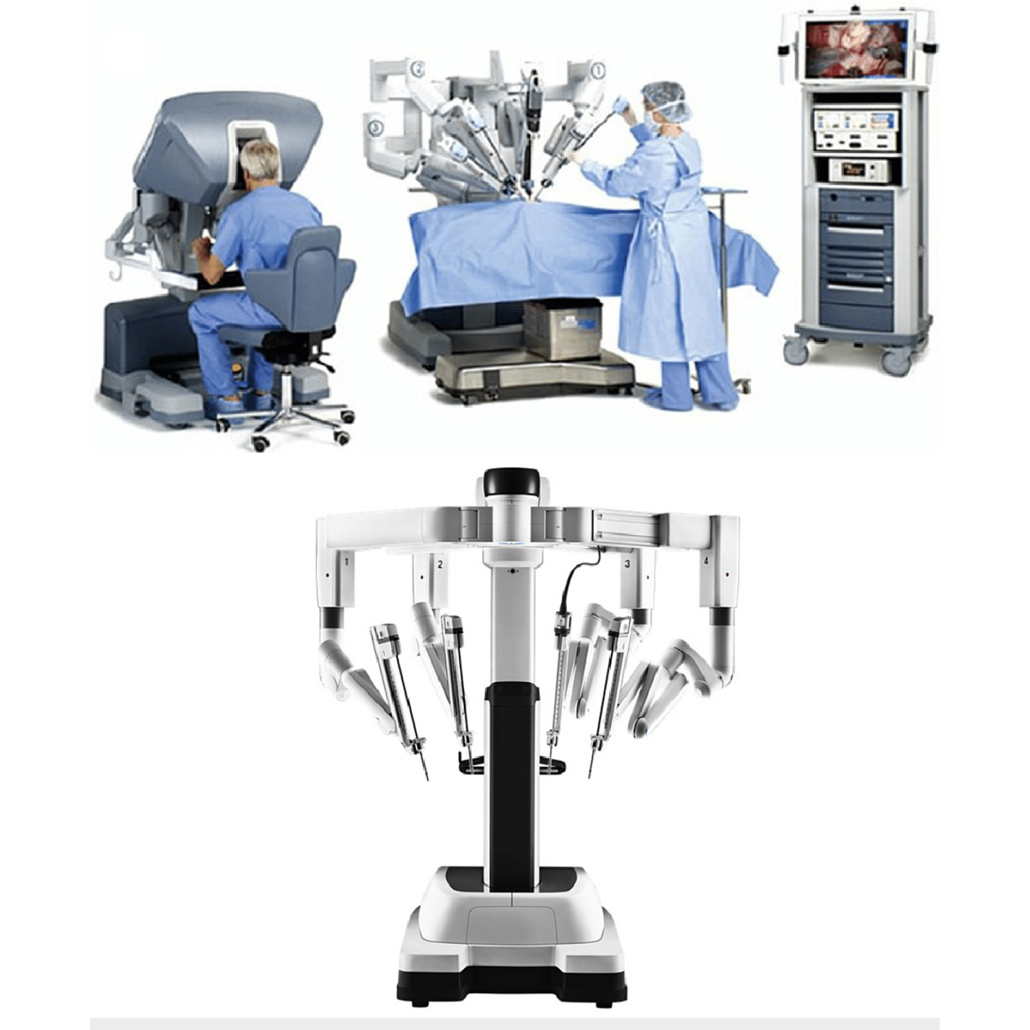
Subsequently a number of other surgical robots have been introduced. Robotic-assisted radical prostatectomy has undoubtedly been made easier to perform with less pain for patients, fewer complications and reduced hospital stay. Robotic-assistance has become a "game-changer" for both surgeons & patients whilst robotic surgery is now widely used for other urological procedures and has been adopted by many other surgical specialties ... once again, though, urologists have led the way!
Additional information
Click on any image below to access more detailed information about individuals featured above, or click here to go to the main History section of this website for more general history content:
|

Charles Huggins
|

Malcolm Bagshaw
|

Andrew Schally
|
|

Hugh Hampton Young
|

Patrick Walsh
|

Mani Menon
|
|
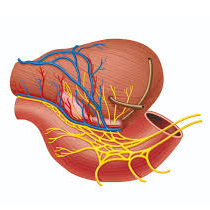
Cavernous nerves
* (image attribution below)
|
|
|
Footnote
|
← Back to BAUS 80th Anniversary